This article provides an overview of root canal treatment and tooth extraction, outlining the factors to consider when deciding between these two dental procedures.
Understanding the Anatomy of a Tooth
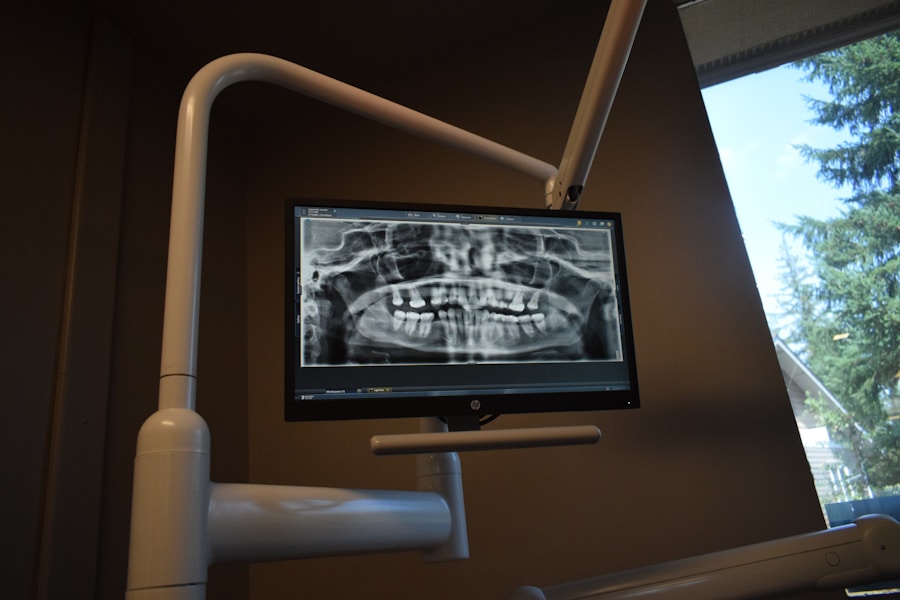
Before delving into the procedures, it is helpful to understand the basic structure of a tooth. A tooth is more than just the visible white enamel. Beneath the enamel lies the dentin, a bone-like tissue. Deeper still is the pulp, a soft tissue containing nerves, blood vessels, and connective tissue. This pulp extends down into the roots of the tooth in channels called root canals. The health of the pulp is central to the decision between a root canal and extraction.
The Enamel: The Tooth’s Protective Shield
The enamel is the hardest substance in the human body, forming the outermost layer of the tooth. Its primary function is to protect the underlying dentin and pulp from decay, bacteria, and physical damage. It is porous and susceptible to acid erosion from food and bacteria.
Dentin: The Supportive Structure
Dentin constitutes the bulk of the tooth, situated beneath the enamel. It is less hard than enamel but still possesses significant strength. Dentin contains microscopic tubules that connect to the pulp, contributing to the tooth’s sensitivity to temperature and pressure.
The Pulp: The Tooth’s Living Core
The dental pulp is the vital component of the tooth. It houses the nerves that provide sensation, the blood vessels that supply nutrients, and lymphatic vessels that help fight infection. When the pulp becomes inflamed or infected, it can lead to significant pain and requires intervention.
When is a Root Canal Necessary?
A root canal treatment, also known as endodontic therapy, is recommended when the pulp of a tooth becomes infected or inflamed. This situation often arises due to deep decay, repeated dental procedures on the same tooth, cracks or chips in the tooth, or trauma to the tooth, even if there is no visible injury. Without treatment, the infected pulp can cause severe pain, swelling, and the formation of an abscess. The goal of a root canal is to save the natural tooth by removing the diseased pulp.
Deep Caries and Pulp Involvement
When cavities are left untreated, bacteria can penetrate the enamel and dentin, eventually reaching the pulp chamber. This leads to infection and inflammation of the pulp tissue.
Trauma to the Tooth
A blow to the tooth, even without fracturing the enamel, can damage the pulp. The trauma can cause the pulp to become inflamed or necrotic (die).
Cracked or Chipped Teeth
Cracks or chips in a tooth can create pathways for bacteria to enter the pulp chamber, leading to infection.
Repeated Dental Procedures
Multiple dental treatments on the same tooth can sometimes irritate the pulp, leading to inflammation or infection over time.
The Root Canal Procedure: A Detailed Look
A root canal treatment is a multi-step process typically performed by a dentist or an endodontist (a root canal specialist). The primary objective is to remove the infected or inflamed pulp, clean and disinfect the root canal system, and then fill and seal it to prevent future infection. While often perceived as a daunting procedure, advancements in dental technology have made it considerably more comfortable and predictable.
Cleaning and Shaping the Canals
After numbing the area and isolating the tooth, the dentist creates an opening in the crown to access the pulp chamber. Specialized instruments are used to carefully remove the diseased pulp tissue from the pulp chamber and the root canals. The canals are then cleaned, shaped, and disinfected to eliminate any remaining bacteria.
Filling and Sealing
Once the canals are thoroughly cleaned, they are filled with a biocompatible material, typically gutta-percha. This material is a rubber-like substance that is sealed into the canals to prevent reinfection. The opening in the crown is then temporarily or permanently sealed.
Restoration of the Tooth
After a root canal, the tooth is often weakened and may require a crown to protect it from fracture and restore its full function. The crown acts as a cap, providing strength and durability to the treated tooth.
When is Extraction Recommended?
Tooth extraction, or the removal of a tooth, is generally considered when a tooth is too severely damaged to be saved by a root canal treatment or other restorative procedures. This can include teeth that are extensively decayed, have advanced periodontal disease, are severely fractured below the gum line, or are impacted (like wisdom teeth) and causing problems. While extraction provides immediate relief from pain and infection, it also leads to a gap in the dentition, which can have subsequent consequences.
Irreparable Tooth Damage
When a tooth is fractured beyond repair, or severely decayed to the point where restoring it would be impractical or impossible, extraction becomes the necessary course of action.
Severe Periodontal Disease
Advanced gum disease can lead to bone loss around the tooth, making it loose and unsalvageable. In such cases, extraction might be recommended to prevent further spread of infection.
Impacted Teeth
Teeth that do not have enough room to erupt properly, such as wisdom teeth, can become impacted and cause pain, infection, or damage to adjacent teeth. Extraction is often the solution.
Orthodontic Reasons
In some orthodontic cases, teeth may need to be extracted to create space for proper alignment of other teeth.
The Extraction Procedure and Its Aftermath
Tooth extraction is a surgical procedure to remove a tooth from its socket in the bone. The method used depends on whether the tooth is fully erupted and easy to access or impacted and more difficult to remove. Post-extraction care is crucial for proper healing and to minimize complications.
Simple vs. Surgical Extractions
A simple extraction is performed on teeth that are visible above the gum line and have intact roots. The tooth is loosened with an instrument called an elevator and then removed with forceps. A surgical extraction is more complex and may be necessary for impacted teeth, broken teeth, or teeth with curved roots. This procedure may involve cutting the gum tissue, removing some bone, and dividing the tooth into smaller pieces for removal.
Healing and Potential Complications
After extraction, a blood clot forms in the socket, which is essential for healing. It is important to avoid dislodging this clot, as it can lead to a painful condition called dry socket. Pain management and infection prevention are key aspects of post-extraction care.
Root Canal vs. Extraction: Making an Informed Decision
Deciding between a root canal and an extraction involves weighing the pros and cons of each procedure in the context of your specific dental health and overall well-being. The primary goal of modern dentistry is to preserve natural teeth whenever possible, making root canal treatment the preferred option in many cases where the tooth is deemed savable. However, there are situations where extraction is the more practical or necessary choice.
Factors Favoring Root Canal Treatment
Root canal treatment is favored when the tooth is structurally sound enough to be restored after the procedure, and when preserving the natural tooth is a priority. It helps maintain the natural alignment of your teeth, prevents bone loss in the jaw, and allows you to continue chewing normally without the need for replacement teeth. A healthy natural tooth is often the best foundation for your bite.
Factors Favoring Extraction
Extraction may be the more suitable option when a tooth is severely damaged, infected beyond the possibility of saving with endodontic therapy, or when the cost of saving the tooth, including subsequent restorations like a crown, outweighs the benefits or is financially prohibitive compared to extraction and a replacement. If the tooth is contributing to ongoing pain and infection that cannot be resolved, removal might be the most straightforward solution.
The Long-Term Implications of Each Choice
Choosing to extract a tooth leaves a gap in your smile and can disrupt the function of your bite. Over time, neighboring teeth may shift into the empty space, leading to misalignment and potential problems with chewing and jaw joint health. This can necessitate expensive orthodontic treatment or the need for tooth replacement options such as bridges, dentures, or dental implants. A root canal, on the other hand, aims to maintain the tooth’s original position and function, avoiding these subsequent issues, though it requires careful consideration of the long-term durability of the treated tooth and the potential need for a crown.
Consulting Your Dentist
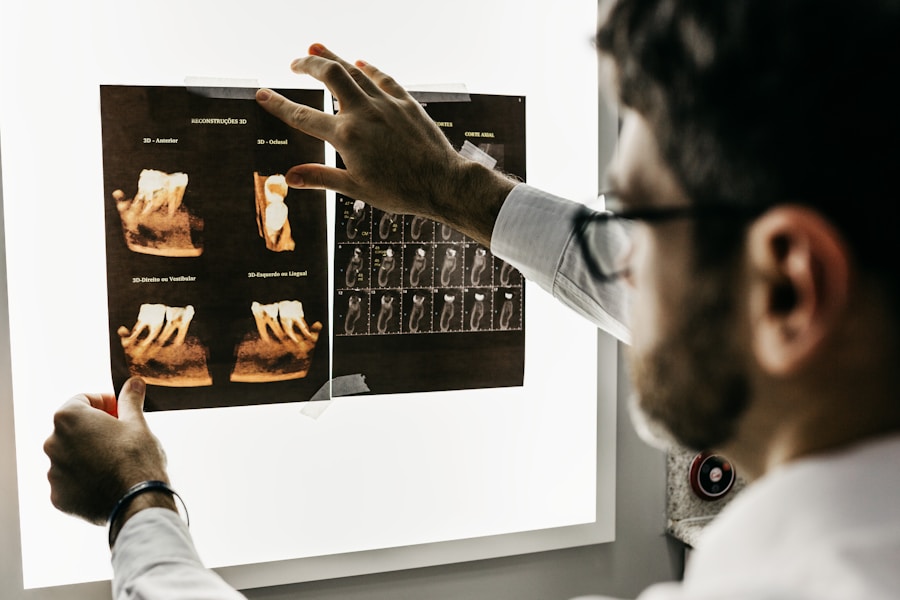
The most critical step in making this decision is to have an open and thorough discussion with your dentist. They can assess the condition of your tooth, take necessary X-rays, and explain the prognosis for both root canal treatment and extraction. They will consider factors such as the extent of decay or damage, the health of the surrounding bone and gums, your overall health, and your financial considerations. Armed with this professional guidance, you can make an informed choice that aligns with your dental health goals.