This is a general article about gum disease and its warning signs. The information provided is for educational purposes only and should not be considered medical advice. Always consult a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Understanding Gum Disease: A Silent Threat
Gum disease, also known as periodontal disease, is a prevalent inflammatory condition affecting the gums and surrounding structures that support the teeth. It is a significant public health concern, often progressing silently in its early stages, making its recognition crucial for effective intervention. This condition can range from mild inflammation of the gums, known as gingivitis, to severe destruction of the tissues and bone that hold teeth in place. The progression of gum disease is primarily driven by bacteria found in plaque, a sticky film that constantly forms on teeth. When plaque is not adequately removed through diligent oral hygiene, these bacteria produce toxins that irritate the gum tissue, triggering an inflammatory response.
The oral cavity is a complex ecosystem, and when the balance of bacteria is disrupted by factors like poor oral hygiene, smoking, or certain medical conditions, harmful bacteria can proliferate. These pathogenic bacteria can then breach the gum’s natural defenses, leading to an infection. Initially, this infection may manifest as gingivitis, characterized by reddened, swollen, and bleeding gums. However, if left untreated, gingivitis can advance to periodontitis, a more serious form of gum disease. In periodontitis, the inflammation extends beneath the gum line, damaging the connective tissues and the alveolar bone that anchors the teeth. This damage can result in the formation of periodontal pockets, which are spaces that form between the gums and teeth, providing a more hospitable environment for bacteria to thrive. As the disease progresses, these pockets deepen, leading to further tissue and bone loss. The stability of the teeth is compromised, and in advanced stages, tooth loss can occur.
The impact of gum disease extends beyond the oral cavity. Research has increasingly highlighted the systemic implications of periodontal infections. The inflammatory mediators and bacteria released from infected gums can enter the bloodstream, potentially affecting other organs and systems in the body. Links have been suggested between gum disease and an increased risk of cardiovascular disease, diabetes complications, respiratory infections, and adverse pregnancy outcomes. This underscores the importance of viewing oral health not in isolation, but as an integral component of overall well-being. Recognizing the early warning signs of gum disease is paramount, as it allows for timely intervention, management, and potentially the prevention of more severe consequences, both locally in the mouth and systemically throughout the body.
The Insidious Nature of Early Gum Disease
Many individuals are unaware they have gum disease because the early stages are often characterized by subtle symptoms that can be easily overlooked or attributed to other minor irritations. This deceptive nature makes early detection a challenge, yet it is precisely during these initial phases that the condition is most manageable and reversible. The primary culprit behind this insidious onset is gingivitis, the precursor to more advanced periodontal disease. Gingivitis is an inflammation of the gums caused by the accumulation of plaque on the teeth. The bacteria within plaque produce toxins that irritate the gum tissue, prompting an inflammatory response.
At this stage, the damage is confined to the gums themselves. The bone and connective tissues that hold the teeth in place remain unaffected. However, even seemingly minor changes in the appearance or feel of the gums can be early indicators. You might notice that your gums appear brighter red than usual, or perhaps they seem a little puffier. The most common and often the first noticeable symptom is bleeding gums. This bleeding typically occurs during brushing or flossing, and a responsible individual might mistakenly believe they are brushing too hard, or that the bleeding is a sign of a minor cut. However, healthy gums should not bleed regularly with gentle cleaning. This bleeding is, in fact, a red flag, a signal from your gums that they are under attack from the bacterial onslaught.
The lack of significant pain in the early stages also contributes to its stealthy progression. Unlike caries (tooth decay), which can cause sharp, throbbing pain once it reaches the nerve, gingivitis is largely painless unless an infection becomes more severe. This absence of discomfort can lead one to believe that everything is fine. Furthermore, the consistent presence of plaque can lead to the subjective feeling of a gritty or rough surface on the teeth, even after brushing. This is due to the ongoing buildup of bacterial film. While this might prompt more vigorous brushing, it often fails to address the underlying inflammation.
The deceptive nature of early gum disease means that neglecting it is akin to ignoring a small crack in a dam; while it may seem insignificant at first, its continued presence allows water pressure to widen the fissure, eventually leading to a catastrophic breach. Similarly, the seemingly minor inflammation of gingivitis, if unaddressed, can create the conditions for the disease to advance, leading to irreversible damage to the supporting structures of the teeth. Therefore, becoming familiar with the subtle signs and understanding their true significance is the first line of defense against the silent invasion of gum disease.
Redness and Swelling: The Gum’s Inflammatory Response
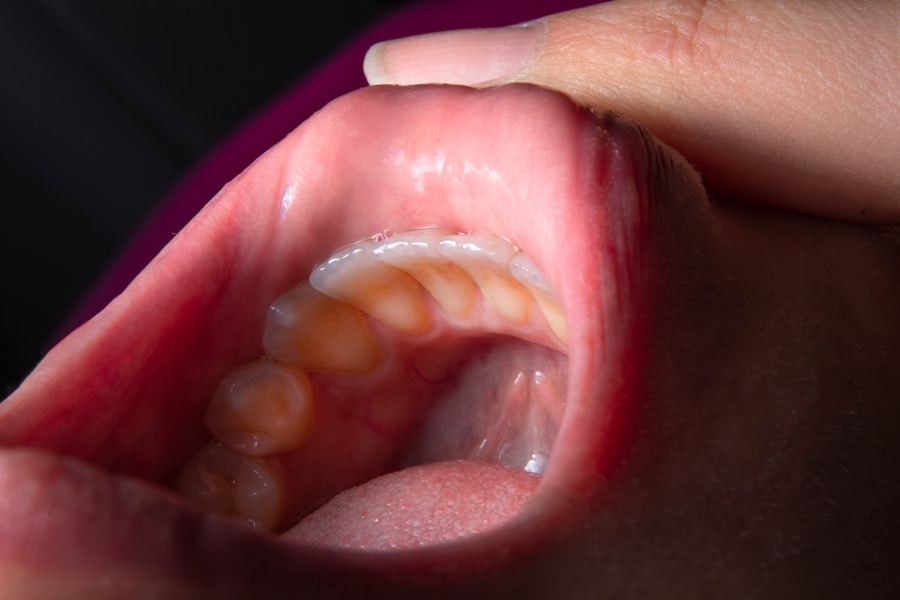
One of the most common and observable warning signs of gum disease is a noticeable change in the color and texture of the gums. Healthy gums typically possess a pale pink hue and a firm, stippled appearance, resembling the skin on an orange peel. This healthy state signifies well-nourished and properly supported gum tissue. However, when bacteria in plaque begin to irritate and infect the gums, the body’s natural inflammatory response kicks in. This response is designed to protect the tissues and fight off the invading pathogens.
The initial manifestation of this inflammation is often a change in color. Your gums may begin to appear redder than their usual pink. This redness can vary in intensity, from a mild rosy flush to a pronounced, angry red. This vibrant color is due to an increase in blood flow to the area. As the blood vessels dilate to deliver immune cells and other defensive agents to the site of infection, the gums take on a more erythematous appearance. This increased blood flow is a direct consequence of the body’s attempt to combat the bacterial toxins and byproducts that are irritating the gum tissue.
In addition to the color change, you may also notice swelling, or edema, of the gum tissue. The gums can appear puffy, enlarged, and lose their characteristic firmness and stippled texture. Instead, they may feel soft and boggy, almost like a waterlogged sponge. This swelling arises from the accumulation of fluid within the tissue spaces as part of the inflammatory process. The body’s immune system sends fluid to the affected area to help flush out toxins and transport immune cells. This combination of redness and swelling is the visual hallmark of gingivitis, the initial stage of gum disease.
It is crucial to understand that these changes are not simply cosmetic. They are concrete signs that your gums are in distress. The inflammation compromises the integrity of the gum tissue, making it more susceptible to further damage. While these signs might seem less alarming than pain or bleeding, they are nevertheless critical indicators that the bacterial imbalance is taking hold. Ignoring this visual warning is akin to dismissing a smoke alarm because you don’t see flames; the signal is there, and it requires immediate attention to prevent a larger fire. Regular self-examination of your gums, perhaps during or after brushing, can help you identify these subtle but significant changes. If you notice any persistent redness or swelling, it is time to seek professional advice.
Bleeding Gums: A Cry for Help
Perhaps the most universally recognized sign of impending trouble with your gums is bleeding. This symptom is often the first and most emphatic signal that something is amiss with your oral health, a loud alarm bell for a condition that may otherwise be quiet. Healthy gums, when subjected to routine cleaning activities such as brushing or flossing, should not bleed. The delicate capillaries within the gum tissue are well-protected when the gums are healthy and firm. However, as plaque accumulates along the gum line, it harbors bacteria that produce toxins. These toxins irritate and inflame the gum tissue, making it more fragile and prone to rupture.
When you brush your teeth and notice blood on your toothbrush or in the sink, it is not a sign that you are brushing too hard. Instead, it is a direct indication that the gum tissue is inflamed and has become compromised. This bleeding is a consequence of the increased permeability of the blood vessels within the inflamed gum tissue. The inflammatory process causes the blood vessel walls to weaken, making them tear easily under normal mechanical stress. Think of it like water seeping through a weakening fabric; the pressure of cleaning is enough to cause a breach.
Similarly, when flossing, you might experience bleeding. Flossing is designed to clean the spaces between teeth, areas where gum disease often begins. The act of inserting the floss can snag on inflamed, swollen gum tissue, causing it to bleed. Again, this is not a sign to stop flossing; rather, it is a sign that you need to address the underlying gum inflammation that is causing the bleeding. In fact, continuing to floss gently but regularly can help to remove plaque from these critical areas and can, over time, help reduce bleeding as the gums heal.
The problem arises when people actively avoid brushing or flossing because they are afraid of causing bleeding. This avoidance is counterproductive and exacerbates the problem. By ceasing to clean these areas, you allow plaque to accumulate further, feeding the bacteria and intensifying the inflammation. This creates a vicious cycle where bleeding leads to avoidance, which leads to more plaque, which leads to more bleeding. It’s like trying to put out a fire by refusing to use water; the problem only gets worse. Recognizing bleeding gums as a symptom, not a cause, is crucial. It’s the body’s way of telling you that the bacterial invasion is causing damage and that intervention is necessary.
Persistent Bad Breath: The Unseen Foul Play
Halitosis, commonly known as bad breath, is a symptom that can affect anyone from time to time. However, persistent bad breath that does not resolve with regular brushing and mouthwash can be a significant indicator of underlying gum disease. This type of chronic halitosis is not merely an inconvenience; it can be the result of bacterial activity within the pockets that form between the gums and teeth as gum disease progresses. The bacteria responsible for gum disease produce volatile sulfur compounds (VSCs) as a byproduct of their metabolism. These VSCs are malodorous, and their presence can lead to an offensive breath odor.
In the early stages of gum disease, such as gingivitis, the increased inflammation and bleeding may contribute to bad breath. The blood in the mouth can create a metallic or unpleasant taste, and the presence of inflamed tissue can provide a more hospitable environment for odor-producing bacteria. However, as gum disease advances to periodontitis, the situation can become more severe. The formation of periodontal pockets, those gaps between the gum and the tooth, creates an anaerobic environment where specific types of bacteria that thrive in the absence of oxygen can flourish. These bacteria are highly efficient at producing VSCs.
These pockets can become reservoirs for food debris and dead cells, which serve as a nutrient source for these odor-causing bacteria. The deeper the pockets, the more difficult it is for even thorough brushing to reach and clean them effectively. The trapped bacteria and their byproducts are then constantly released into the oral cavity, leading to a persistent and often offensive smell. Mouthwashes may provide temporary relief by masking the odor, but they do not address the root cause of the problem, which lies in the submerged bacterial colonies within the periodontal pockets.
Think of persistent bad breath in the context of gum disease as the unseen smoke from a smoldering fire. While you might not see the flames, the smoke is a clear indication that something is burning and needs to be extinguished. The odor is the invisible evidence of a bacterial battle raging in your mouth. Ignoring this persistent symptom is akin to ignoring the smell of smoke; it suggests a deeper problem that requires investigation. If you find that your breath remains unpleasant despite diligent oral hygiene, it is a strong signal to consult a dental professional. They can examine your gums, identify the presence of periodontal pockets, and determine if gum disease is the culprit behind your persistent halitosis.
The Role of Bacteria in Odor Production
The mouth is a complex ecosystem teeming with a diverse population of microorganisms. In a healthy mouth, there is a balance of bacterial species, most of which are harmless and even beneficial. However, factors such as poor oral hygiene, diet, and certain medical conditions can disrupt this balance, leading to the overgrowth of pathogenic bacteria. These harmful bacteria are the primary drivers of gum disease and, consequently, are also responsible for the production of unpleasant odors.
When individuals neglect their oral hygiene, plaque, a sticky film composed of bacteria and food particles, accumulates on the teeth and along the gum line. The bacteria within this plaque consume sugars and other nutrients from food debris. As a metabolic byproduct of their activity, they release certain compounds. While some of these byproducts are neutral, others are volatile sulfur compounds (VSCs), which are known for their foul smell, often described as rotten eggs or sulfurous.
The specific types of bacteria involved in gum disease, particularly those found in periodontal pockets, are particularly adept at producing VSCs. These bacteria often thrive in low-oxygen environments. Periodontal pockets, by their very nature, create such an environment. Food particles and debris trapped within these pockets become a breeding ground for these anaerobic bacteria. As they break down proteins and other organic matter, they release significant amounts of VSCs directly into the oral cavity.
The continuous production and release of these malodorous compounds are what lead to persistent bad breath. While brushing mechanically removes some of the plaque and associated bacteria, it may not be sufficient to eradicate the deep-seated bacterial colonies within the periodontal pockets. Similarly, the chemical compounds in some mouthwashes may temporarily reduce the number of odor-causing bacteria or mask the smell, but they do not eliminate the underlying infection. Therefore, chronic halitosis, in the absence of other obvious causes like dietary indiscretions or sinus issues, should be considered a crucial warning sign that the bacterial imbalance in your mouth has reached a point where it is actively contributing to the decay of your oral tissues. It is the unseen damage manifesting as an audible, albeit olfactory, warning.
Receding Gums: The Slow Retreat of Protection
Receding gums, also known as gingival recession, is a process where the gum tissue surrounding the teeth gradually pulls back or shrinks, exposing more of the tooth’s root and often the underlying bone. This phenomenon is a significant warning sign of gum disease, indicating that the supportive structures of the teeth are being compromised. While some degree of recession can occur due to factors like aggressive brushing or the natural aging process, significant and rapid recession is often a direct consequence of untreated periodontal inflammation.
As gum disease progresses, the inflammatory process can lead to the destruction of the connective tissues that bind the gums to the teeth and the underlying bone. The body’s immune response, aimed at fighting the infection, can inadvertently begin to break down these essential supporting structures. This breakdown causes the gums to detach from the teeth and retract. Initially, the recession might be subtle, with only a small portion of the root becoming exposed. However, as the disease continues unchecked, the gums can recede further, leaving significant portions of the tooth’s root bare.
The exposure of the tooth root is a critical concern for several reasons. Tooth enamel, the hard outer layer of the tooth crown, is designed to withstand the conditions of the oral cavity. However, the cementum that covers the tooth root is much softer and more vulnerable to erosion and decay. Once the roots are exposed, they become susceptible to increased sensitivity to hot, cold, and sweet stimuli. This sensitivity can be an early indicator for individuals that their gums are receding.
Furthermore, receding gums create deeper pockets between the teeth and gums, providing more space for plaque and bacteria to accumulate. This exacerbates the cycle of inflammation and destruction, leading to further recession and bone loss. The teeth may also appear longer than usual, and the overall appearance of the smile can be altered. In advanced cases, the loosening of teeth can occur as the supporting bone is lost, eventually leading to tooth mobility and potential tooth loss.
The progressive nature of gum recession is a stark reminder that the foundations of your dental health are eroding. It’s like observing the shoreline slowly being eaten away by the tide; while the process may be gradual, the relentless erosion signifies a loss of stable ground. Recognizing receding gums as more than just an aesthetic concern is vital. It is a powerful indicator that the protective barrier around your teeth is weakening, and urgent professional attention is needed to halt its destructive course and preserve the integrity of your smile.
Increased Tooth Sensitivity: The Exposed Vulnerability
One of the more uncomfortable and directly experienced warning signs of gum recession, and by extension gum disease, is increased tooth sensitivity. As the gums recede, they expose the underlying tooth root. Unlike the crown of the tooth, which is covered by a thick layer of protective enamel, the root surfaces are covered by a thinner layer of cementum, which is softer and less resistant to wear and decay. Beneath the cementum and enamel are the dentin tubules, which are microscopic channels that lead directly to the tooth’s pulp – the nerve center.
When these dentin tubules are exposed to the external environment, stimuli that would normally pass harmlessly over the enamel can now penetrate to the nerve, triggering pain or discomfort. This sensitivity can manifest in various ways. You might experience a sharp, sudden twinge when consuming hot or cold beverages and foods. Sweet foods and drinks can also elicit a painful response. Even breathing in cold air can sometimes cause a jolt of sensitivity.
This heightened sensitivity is the tooth’s way of signaling distress. It’s like a nerve ending that has been stripped of its protective covering and is now reacting to every brush of the wind. The exposed root surface acts as a direct conduit for temperature changes and the chemical stimuli from certain foods and drinks to reach the nerve endings within the pulp. This discomfort can be quite disruptive, impacting your ability to enjoy everyday pleasures like eating and drinking.
While increased tooth sensitivity can have other causes, such as tooth decay or a cracked tooth, when it is accompanied by other signs of gum disease, such as redness, bleeding, or visible recession, it becomes a particularly strong indicator of periodontal issues. Many individuals might attribute this sensitivity to brushing too hard or to the use of whitening products, and they may switch to desensitizing toothpaste. While these toothpastes can offer some relief by blocking the dentin tubules, they do not address the fundamental problem of gum recession and the underlying cause of the sensitivity.
Therefore, persistent or new-onset tooth sensitivity, especially when it occurs in conjunction with other oral health concerns, should not be dismissed. It is a clear signal that the protective layers of your teeth are being compromised, and that the health of your gums is likely at stake. Ignoring this discomfort is akin to ignoring an exposed electrical wire; it poses a risk of significant damage if left unaddressed. Seeking professional dental evaluation is crucial to determine the cause of your sensitivity and to implement appropriate treatment to safeguard your teeth and gums.
Loose or Shifting Teeth: The Foundation Crumbles
Perhaps the most alarming and definitive sign of advanced gum disease is the development of loose or shifting teeth. This symptom signifies that the underlying structures supporting the teeth – the periodontal ligaments and the alveolar bone – have been significantly compromised by the ongoing inflammatory process. In healthy mouths, these structures act like strong anchors, holding the teeth firmly in place. However, as gum disease progresses into its more severe stages, periodontitis, these anchors begin to erode.
The chronic inflammation associated with periodontitis leads to the destruction of the periodontal ligament, the fibrous connective tissue that attaches the tooth root to the bone. Simultaneously, the alveolar bone, the bony socket that cradles the tooth, also undergoes resorption – a process where the bone tissue is broken down and reabsorbed by the body. This destruction of both the ligaments and the bone progressively weakens the stability of the teeth.
Think of teeth as being rooted in the ground. In healthy gums, the roots are firmly embedded in a substantial amount of stable soil. As gum disease progresses, this soil erodes, and the roots become loosened, making the teeth wobbly. Initially, you might notice this loosening only when you bite down, or you might feel a slight degree of movement in a tooth that was previously rock-solid. This sensation can be subtle at first, and some individuals tend to dismiss it as temporary or due to a recent hard bite.
However, if the underlying gum disease is not addressed, the loosening will become more pronounced. Teeth may begin to shift their positions in the mouth. You might notice changes in your bite, where your upper and lower teeth no longer align properly. This shifting can lead to further complications, such as increased pressure on certain teeth, which can accelerate bone loss and exacerbation of tooth mobility.
In the most advanced stages of periodontal disease, teeth can become so loose that they are easily moved with the fingers, or they may even fall out on their own. This dire outcome is the ultimate consequence of neglecting the warning signs of gum disease. It represents a complete failure of the supporting structures to maintain the integrity of the teeth.
The development of loose or shifting teeth is not a symptom that can be ignored or treated with home remedies. It is a critical indicator that the structural integrity of your smile is at severe risk. This is the point where the foundations have crumbled, and immediate, professional intervention is paramount to attempt to salvage any remaining support and prevent further loss. It is a stark reminder that the silent invasion has now manifested in a way that threatens the very permanence of your teeth.
The Impact of Bone Loss on Tooth Stability
The stability of your teeth is intrinsically linked to the health and integrity of the surrounding bone and connective tissues. When gum disease progresses to periodontitis, the primary mechanism of tooth loosening is the loss of this crucial supportive infrastructure. The alveolar bone, which forms the socket in which each tooth rests, is a dynamic tissue that is constantly being remodeled. However, in the presence of chronic inflammation caused by bacterial infection, this remodeling process becomes destructive.
Inflammatory mediators released by the body’s immune system, in its fight against the bacteria, trigger osteoclasts – specialized cells responsible for breaking down bone tissue. These osteoclasts are activated in large numbers around the infected gums and bone, leading to a process of bone resorption. Essentially, the body begins to break down the very bone that holds your teeth in place.
Simultaneously, the periodontal ligament, a network of strong collagen fibers that connects the tooth root to the alveolar bone, is also attacked by the inflammatory process. These fibers become degraded, and their ability to anchor the tooth securely is diminished. As more and more of these anchoring fibers are destroyed, and as the bone socket is resorbed, the tooth loses its firm foundation.
The consequence of this combined loss of bone and ligament support is tooth mobility. The tooth is no longer held firmly in its socket. Imagine a flagpole that has been significantly weakened at its base; it can sway and become unstable. Similarly, as the bone and ligament support for a tooth erodes, the tooth becomes loose. The degree of looseness is directly proportional to the extent of bone loss.
Early bone loss may result in only slight, imperceptible movement. However, as the disease advances, the bone loss becomes more significant, leading to noticeable wobbling and eventually severe mobility. In severe cases, the bone loss can be so extensive that the tooth is no longer adequately supported, and it may become loose enough to be extracted or even fall out spontaneously.
The irreversible nature of significant bone loss makes it imperative to address gum disease at its earliest stages. While some treatments can help to halt the progression of bone loss and even regenerate some lost bone in specific circumstances, extensive bone destruction cannot be fully reversed. Therefore, recognizing any degree of tooth looseness as a red flag for severe underlying bone loss and immediate professional intervention is essential to preserve your natural teeth and the structural integrity of your jaw.